Treat the Patient, Not the X-rays or Scans
I recently wrote an article describing the total knee patient who was unhappy with his or her surgical result, even though the X-rays and other studies appeared satisfactory. These types of patients are frustrated and describe “going from doctor to doctor” only to be told that knee “looks good” but to them, “it feels bad.” In that article, I describe how common this is – some series report that 20% or more of patients who have had a knee replaced aren’t satisfied with the result. I also see patients who’ve undergone total hip replacement and have similar woes even though their X-rays look good.
In this article I will discuss the patient who has significant disability from a hip or knee, but whose workup either is not definitive or doesn’t appear “severe enough” to warrant joint replacement. Recommending a joint replacement for an elderly patient who has severe hip or knee symptoms (pain, limitations in activity, deformity), a “positive” hip or knee exam (when the hip or knee is moved or challenged it hurts or is unstable) and who has X-rays which show advanced degenerative osteoarthritis, is relatively straight forward. Everybody agrees that these are the perfect candidates for joint replacement.
It’s not so straightforward when the patient is very young or when the symptoms and limitations seem out of proportion to the appearance of the X-rays. There are many patients like this and they come to me frustrated, and many times depressed. I’ve heard them describe their plight with phases such as, “giving up,” “resigned to inactivity,” “no quality of life,” or “life passing them by.” One of my favorites that I heard just last week was, “I feel like I’m in a black hole and don’t know what to do next.” I think many of us can relate to that.
When I approach these patients, I do so as a clinician. In our modern day world, we place tremendous emphasis on imaging studies and radiologist reports. They are very helpful, but don’t capture the whole picture. It’s critical that we as physicians truly listen to our patients to understand and assess the nature of each individual’s symptoms by asking the right questions. For example, when did the symptoms start, what makes them worse, or what relieves the symptoms (i.e., ice, rest, sitting)? Where exactly is the pain and does it radiate? Is the pain dull, constant, sharp and episodic, etc.? Does pain awaken them at night? Are they unable to find a comfortable position? Does the joint lock or give way? Can they trust the limb when they walk? Can they navigate stairs? If so, is it more difficult going up or down steps? Are they limping? Of course, these are just examples but like a good news reporter, it is important as a clinician to keep an open mind. Also, we must consider other etiologies such as referred pain from back trouble.
It’s also vital for me to understand what’s already transpired. What other doctor’s have they seen and what studies or therapies have they had? The consequences of these therapies must be scrutinized. Were they prescribed NSAIDs? If so, which ones and how long did they take them – on a short-term schedule, indefinitely or PRN (as needed)? Are they taking other meds such as narcotics or muscular relaxers? Did they have physical therapy? Did the therapy help and if so for how long and how much? Or, did the therapy exacerbate the condition?
With the proliferation of pain management physicians, more and more patients are having their joints injected. It is critical to know if an injection was given intra-articularly (within the joint space) or administered extra-articularly (outside the joint space). And, what was injected (i.e., a steroid with a local anesthetic, Hyaluronic acid, PRP, growth hormone)? Did the injection(s) help?
Many initially will tell me that injections did not help, but with further questioning, I learn that they may have gotten some degree of relief at least temporarily. If they tell me they felt relief for only an hour or two, then the injection can be considered a therapeutic failure, but diagnostically gives me confidence that the problem truly is emanating from pathology within the joint and not from an extra-articular source or referred pain.
Many patients whom I see have had prior hip or knee surgeries. Knee patients might describe an ancient high school sports injury and possibly had surgery well before our modern day arthroscopic techniques. Many have had a prior knee or even hip scope. If images were taken during those procedures, reviewing them can be invaluable. Some patients with hip symptoms have been evaluated for a hip arthroscopy but advised against it because of underlying dysplasia (a shallow socket) or arthritis. This is important history.
For patients presenting with symptoms that are debilitating, but have X-rays that show only minimal pathology or no obvious pathology, the physical exam is critical. In today’s world, technological advances now allow the visualization of the skeleton (X-rays and CT) and the soft tissues (MRI) with tremendous precision. This can result in much-less emphasis and time being spent on the physical exam. I believe this is a mistake, particularly in this population of patients for whom the pathology is not so “clear cut” and who are very symptomatic with their hips or knees, yet their imaging studies don’t reveal the full nature of the problem.
By constantly performing physical exams, it builds a physician’s skills in recognizing and diagnosing the problem and also the confidence to act on the exam when “all the stars don’t line up” (i.e., a positive history, physical exam and X-rays or scans).
Advising a very young person to proceed with a joint replacement is a particularly difficult decision. Historically, total joint replacements were reserved for elderly or sedentary patients because their longevity was limited and the results when revision surgery was required weren’t as predictable or good. Today, so much has changed. The whole operation, from beginning to end, is greatly improved in almost every regard. The wear characteristics of the bearing of our prosthetics are a magnitude better than what were available only 12-15 years ago. The prosthetic designs and the techniques to implant them are much more precise and refined and we now have extensive experience performing revision surgeries. New techniques and wonderful modular prosthesis now are routinely available to “customize” the new implant intra-operatively, resulting in predictable and excellent results.
Still, the decision to advise young patients (20s or 30s) to have a joint replacement is not an easy one. The hope and expectation is they will live another 50 or 60 years and I don’t believe that present-day prostheses will last that long. Also, historically total joint replacement prostheses have survived longer in older people than the very young because they tend not to be as active or vigorous. This is particularly true with young males who have the worst longevity tract record. Despite these facts, there are times when recommending a joint replacement to someone of a young age is appropriate and in my opinion “the right thing to do.”
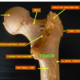
What prompted me to write this blog were several patients I’ve seen in just the last few weeks and I thought I would share their stories. Yesterday, I re- evaluated a 32-year-old nurse who had fractured her hip (femoral neck stress fracture) 10 years prior when she was in Army boot camp. She was treated with pins and the fracture appeared to have healed but she never did well. Over time, it became apparent that the blood supply to her femoral head was interrupted resulting in her femoral head dying and then collapsing (AVN). She quite simply was “broken.” Although she had made it through nursing school, she had a horrible limp, contractures and pain. She was so young and said, “No one would operate on me.” I removed her pins (which she kept as a souvenir) and performed a total hip replacement. Yesterday she returned with her fiancée, a year and a half after her surgery, smiling and walking beautifully.
Also recently, I met a 47-year-old successful property manager who had become so disabled from pain in both of his hips he couldn’t sit and he told me he had “lost all quality of life.” His X-rays demonstrated a lack of full femoral head coverage (he had mild hip dysplasia) but with only subtle joint space compromise. His MRIs demonstrated a torn labrum with mild underlying arthritis. He had been told he probably wouldn’t do well with a hip arthroscopy and then tried every conservative treatment in the book. In spite of his relatively “benign” X-rays, I replaced both of his hips in a staged fashion. He recently returned to my office and told me that I had, “given him back his life.” He reminded me of something I had told him, “I don’t treat scans; I treat patients.”
This week, an 80-year-old woman returned just six weeks after her hip replacement. She was very grateful and thanked me for “listening to her.” When she first presented, her pre-op X-ray did not show much in the way of osteoarthritis but her history and symptoms all were consistent with hip disease: she had a positive hip exam and a pain injection test relieved all of her symptoms, but only temporarily.
Finally, again this week, I performed a medial unit-compartment knee replacement on a 43-year-old, very active but markedly overweight woman who just three weeks prior had a total knee replacement performed on her other knee. She had been a high-level gymnast during her teens and 20s and over the years had become more and more disabled with pain from both of her knees.
As her knees became more painful and limiting, she stopped exercising and gained a lot of weight. She told me she felt like she was in a “catch 22.” The knee on which I performed the total replacement had undergone a recent scope and her symptoms worsened after the procedure.
Her X-rays showed some arthritis bilaterally, but not advanced or “bone on bone.” At time of the operation, I ascertained much more severe arthritis in both of her knees than I would have predicted from her X-rays alone. She put a big smile on my face when I walked into her hospital room this past Thursday morning. Having only replaced her knee the day before, she was out of bed, dressed and making her own bed. Please understand that I don’t usually see this from patients still in the hospital. She told me she’s a worker. And, she too expressed her gratitude.
We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4575 or by email at LeoneCenter@Holy-cross.com.








Very important post here! It’s amazing how uncommon treating a patient has become. Especially when it comes to things like pain, you really need to listen to the patient about what is going on. Thanks for sharing your insight!
Thank you, Jordan.
Thank you for this post!!! I am in a similar quandry.
I’m 59 and have had a labral tear in my hip for the last 6 years. My current sports med. doc is having a cartilage mapping MRI done on my hip to see if the cartilage damage has worsened to the point where he might feel OK referring me to a THR specialist. X-rays show some sclerosis and that’s it; cortisone injections are not working anymore; NSAID’s help a lot but my stomach rebels (even w/ nexium).
Have been told by one THR guy already ‘yeah, unfortunately there are people like you in the ‘gray’ area, go find something else to try.
I am totally unwilling to try an arthroscopy, altho I DO meet the insurers criteria for that. I had that done on the other hip and was bone-on-bone 6 months later.
I feel that a lot of this is being driven by insurers..e.g. there is a checklist that you seem to have to meet before they are willing to accept that a hip replacement is actually necessary (cost savings?).
For some of us, it seems that we would not be able to get a replacement unless totally debilitated, and at the point where we would have difficulty getting full function back.
Dear Kim,
Thank you for sharing your thoughts. It sounds to me as if you would benefit immensely from THR. You need to find an orthopedic surgeon who will treat you and not your X-rays. If you know you’re not going to have an arthroscopy, then more expensive “cartilage MRI scans” aren’t necessary.
I wish you a full recovery.
Dr. William Leone
We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4584 or by email at LeoneCenter@Holy-cross.com. General comments will be answered in as timely a manner as possible.
Dr. Leone..
I had a total knee replacement 10 years ago, I hurt my knee in the spring and after months of X-rays, ct’s etc I was told I had probably dislocated my replacement. It was very painful and making loud “clicking noise” with most movements. Months later I finally found a doctor who would do a revision, and I had the revision 6 weeks ago. It is still making the “clicking noise” and painful when it does, however I can now walk without (much) pain.
I was just at my 6 week follow up with the orthopaedic surgeon, he said he has know idea what is making the noise, he said he did the replacement and it was so bad he could just lift my old replacement out. However, he didn’t change the plastic lining(why I don’t know). He said it looked ok.
Could my “clicking” becoming from the lining catching? He doesn’t want to do more surgery and just wants to wait and see, says it’s too close to go back in.
Thoughts??