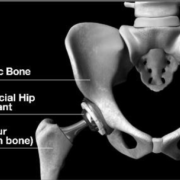
Frequent Reader Questions about Hip Dislocations and Problems
In my last Q&A blog post, I shared some of the most common reader questions about knee replacement surgery. Again, I will use a Q&A format to share some of the most-frequently asked questions and concerns relating to a hip dislocation or hip subluxation, a condition in which the hip joint is partially, but not fully, dislocated.
I will link back to respective blog posts where applicable.
Thank you for your readership and my hope is that you will benefit from this hip Q&A.
Anterior Hip Replacement
Q: I had out-patient anterior hip replacement surgery a few months ago. After being prescribed blood thinners for a week my doctor recommended switching to aspirin. Everything seems fine, I was walking and climbing stairs, but after 10 days I experienced an excruciating subluxation of the joint. My hip has subsequently subluxed more than a dozen times and I continue to be unstable on one leg. Also, since surgery, my knee has been bad as well. My doctor suggested I wait until the four month mark before doing anything further but I am concerned that the joint is not properly aligned or that the wrong size was used. What do you recommend?
A: When your hip joint subluxes, the ball is leaving its normal and intended position which is in the center of the prosthetic socket and raising up to the rim or beyond, then it fortunately falls back into position. Components that are not optimally positioned or related to each other is a common cause of hip subluxation or dislocation. There are other causes such as retained soft tissue or bone which is impinging with certain hip positions, resulting in the ball being levered out of the socket. You need to pay attention to the activities you are doing, i.e. during walking or pivoting or the position your leg is in when the subluxation occurs and avoid these if possible. If despite your precautions to prevent, your hip continues to sublux, you most likely will require further surgery to correct. If this had occurred only once or twice and you could prevent it from happening again, then the hope would be that the tissues which surround your hip would heal, creating a complete and stronger capsule and provide you with greater stability over time. The fact that your hip has subluxed “over a dozen times” suggests you have a mechanical problem which may require surgical correction. I wish you a full recovery.
Q: I had an anterior total right hip replacement less than six months ago but four days after surgery I was rushed to the emergency room with a loose and rotated acetabulator component and underwent revision surgery within the week. The surgeon increased the size to fit a larger acetabular cup for a more stable bite. Two screws were placed where no screws were placed during the first surgery. I had physical therapy and was walking unassisted and feeling great but seven weeks later my right hip dislocated when I was standing on a slight incline and I fell, requiring mild sedation to fix the dislocation.
X-rays later showed an increased abduction angle on the cup but no gross loosening. I was instructed to start activities while being monitored to make sure my implants did not shift further. My hip dislocated after one week later and my orthopedic surgeon suggested a third surgery to tilt the cup down to help prevent additional dislocations. I’m nervous and want to take a conservative approach as I do not want to have yet another surgery with further potential complications. My question is do I have a malalignment where surgery is required or through time will my muscles get strong enough to hold everything in place where surgery is not needed? Was the cup initially not installed on the right angle?
A: I think there is still a very high risk of further dislocation. Your description of your hip dislocating while you were standing suggests it dislocated anterior or in front of your socket. It is very difficult to teach someone to guard against further anterior dislocation because it is often induced during activities or motions which occur during everyday activity, such as pivoting while standing, or laying on your back in bed when your foot rotates out. Without continued dislocations the surrounding soft tissues should heal and your chance of it happening again diminishes. If you are comfortable being “careful” and hoping your hip will not dislocate again, then this is reasonable. On the other hand, if you feel it’s just not stable or you are so frightened that it will happen again that you are paralyzed, then I would suggest proceeding with further revision surgery.
Q: I’m in my early 40s and underwent an arthroscopy for a labral tear and also had a femoral neck shaved and cyst removed. My first consult was with a surgeon who did not repair torn labrums and I was referred to another practice. I had a cortisone injection and they also performed the initial x-ray and arthrogram for diagnosis of labral tear and dysplasia. I had a surgical consult with surgeon who could repair my labrum but did not review x-ray, only arthrogram, and did not seem to be concerned with the dysplasia. Eight weeks after my post-op, it was determined that the arthroscopy resulted in accelerated arthritis, bone-on-bone with a frayed (formerly “repaired”) labrum. Is my only course of action now a THR? I can no longer walk without assistance and am in constant excruciating pain.
A: In all probability you will greatly benefit from total hip replacement. My recommendation would be to focus on finding an orthopedic surgeon who you trust to perform the surgery and care for you. Mentally and physically prepare pre-operatively and then fully rehabilitate afterwards to “get your life back.”
I’m sure that your physicians who tried to help you did their very best to relieve your pain and preserve your joint without total replacement. Sadly, it appears to have failed. You should feel good that you did everything within your power to recover. Now go on with a positive attitude and a great prognosis for the future. I would not look backward.
We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4575 or by email at LeoneCenter@Holy-cross.com. General comments will be answered in as timely a manner as possible.