- Symptoms of Hip Pinning Failure
Pain After a Hip Fracture
Groin pain is a classic symptom for hip disease. While it is true that not everyone who has hip disease has groin pain and not all groin pain originates from hip disease, when someone is experiencing pain in their groin, an underlying hip etiology does need to be considered.
Commonly, individuals who develop hip arthritis, that is, the cartilage space between their femoral head and socket (acetabulum) wears away will develop groin pain. Many times they also have other accompanying symptoms such as pain that radiates down the front of their thigh towards their knee, pain that radiates to the outside or even back of their hip, and occasionally just pain in their lower thigh and knee without groin pain. Lower thigh or knee pain which is caused by a problem with the hip joint is commonly called “referred” pain.
When someone breaks or fractures their hip, this refers to a fracture occurring through their upper thigh bone or femur. If the break occurs within the hip joint capsule, then it typically occurs through their femoral neck. This is the part of the bone that joins the hip ball or femoral head to the upper part of the femur. Historically, femoral neck fractures have been problematic because they often don’t heal or later collapse. If the break occurs through the femoral neck but the bone does not displace or the neck doesn’t displace very much, then many times an attempt is made hold the broken neck fragments in that position using “pins” (actually these are bone screws) to prevent more movement and promote fracture healing. If the fracture through the femoral neck results in significant displacement of the femoral neck and ball from the shaft, then many times the surgeon will choose to replace the broken upper part of the femur (replace the ball and neck) with a prosthesis, rather than trying to put the broken pieces back into an anatomic position and “pin” the fracture.
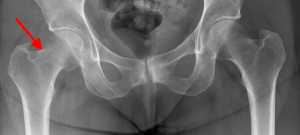
Nondisplaced Femoral Neck Fracture
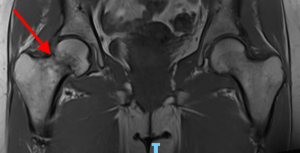
MRI of Nondisplaced Femoral Neck Fracture
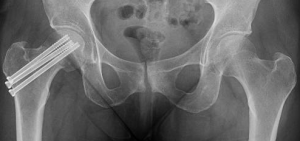
Pinning of Neck Fracture
In an older individual with a femoral neck fracture, there is a stronger tendency to replace the broken ball and neck rather than try and repair it. In a younger individual or if the neck fracture is not displaced, then there is a tendency to “pin” the fracture with the hope that the fracture will heal. The thought process is that it is always better to have your own hip (i.e. get the bone to heal) rather than an artificial one. If the fracture will heal and ultimately results in the person becoming pain free with full return of function. In a very young person with a femoral neck fracture, the decision still might be made to “pin” the fracture even if it is displaced, recognizing there is a high likelihood it may fail and additional surgery in the form of removing the pins and performing necessary THR later. Younger individuals have better healing potential than older people, so the fracture is more likely to heal in younger individuals.
If someone breaks their hip, the fracture can also occur just below the femoral neck and outside of hip joint capsule. This is referred to as an “intertroch fracture” or intertrochanteric fracture. The upper part of ones femur, which is just below the femoral neck and outside of hip joint capsule, is the intertrochanteric femur and includes the greater trochanter and lesser trochanter. While these fractures tend to result in more blood loss and potential for lower leg shortening with external rotation after the fracture, the intertrochanteric boney fragments that make up the fracture are attached to muscle, unlike the neck fracture which is surrounded by
fluid within the hip joint capsule so tends to heal. These fractures often heal but with leg shortening and increased external rotation. These intertroch fractures are usually treated with an attempt to put the bone fragments back into anatomic alignment (called a reduction) and then “pinned”.
While the “pins” to internally fix a femoral neck fracture typically are hollow screws, the “pins” to internally fix an intertrochanteric fracture are much more substantial. Imagine a very large screw being placed up the femoral neck and anchored well into the femoral head. The shank of this “lag screw” is assembled through a hole in a rod that is placed down the medullary canal of the upper femur or though the “barrel” of a plate which is attached to the side of the upper femoral shaft with screws. Both contraptions are designed to allow the smooth shank of “lag screw” to slide so the fracture fragments compress and hopefully promotes fracture healing.
If someone develops groin pain after breaking their hip and having their hip “pinned”, it might be caused by a number of different problems. If the groin pain occurs early after the hip fracture and surgery, it may be from injury to local soft tissue caused by the trauma that led to the fracture or the surgery itself. Blood in the joint and surrounding soft tissues can cause pain. We can see the broken bones on an X-rays but imagine the surrounding soft tissue is also partially torn and bleeding. I would expect this early post-op groin pain to get better with time and hopefully resolve as the fracture and soft tissues go onto heal with hip function restored.
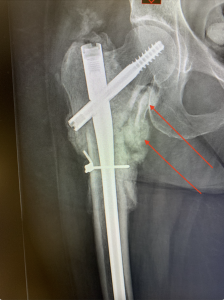
Intertroch hip fracture with controlled collapse with healing. Exuberant bone healing causing impingement and groin pain.
If groin pain is present very soon after surgery and does not get better or even gets worse with time, this is a concerning sign that there is a problem. If may be from the fracture fragments not being solidly fixed or stable after “pinning” so the fragments continue to move resulting in pain. It may be that the “pins” are not solidly fixed in the bone, hence moving and can cause pain. Sometimes we see progressive “pin” or hardware migration or even “cut out” from the bone. Sometimes the pins migrate into the joint space as the bone around the pin collapses, which destroys the hip joint cartilage and results in groin pain. Sometimes the pins migrate outside of the bone and irritate soft tissue which can also cause hip symptoms.
Early groin pain that worsens with time can also be caused by the collapse of the fracture, resulting in boney fragments impinging against the hip socket or acetabulum. Pain occurs with hip movement or when the hip joint is in certain positions which cause the boney fragments to bang together. This can occur even if the fracture does heal and the “pins” remain stable in the bone. I see this more typically with intertroch fractures that go onto heal, but with continued pain.
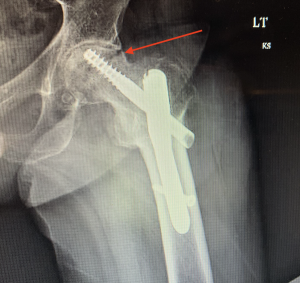
Healed intertrochanteric fracture with delayed segmental AVN with collapse, causing arthritis and groin pain.
Sometimes patients will develop groin pain after a hip “pinning” because the blood supply to their natural hip ball or femoral head is lost. This is referred to as “osteonecrosis” or “avascular necrosis (AVN)”. Bone is a living organ that requires oxygen via blood supply to live. When the oxygen supply is disrupted, areas of bone that comprise the femoral head dies. Our bodies try to heal the area of dead bone by growing new blood vessels which facilitate the removal of the dead bone and lay down new bone. We call this process “creeping substitution”. The new bone being deposited is soft (not yet mineralize) so vulnerable to collapse. So, if the bone that died within the femoral head is in a critical weight bearing position of the head or is a large percentage of the head, then during this time the head is vulnerable and could collapse. The collapse of the femoral head is a “new fracture” and often causes groin pain. The ball is now not round. The overlying cartilage is not supported. Hip joint arthritis then develops as the now flattened, partially collapsed femoral head moves in the socket, resulting in cartilage break down. The resulting hip arthritis often causes groin pain.
While this complication of the femoral head losing its blood supply resulting in collapse classically occurs more frequently after a femoral neck fracture, it can also occur after an intertroch fracture. AVN can occur soon after a hip fracture is “reduced” and “pinned”, but more commonly it is a complication that occurs later. Later can mean six months after the fracture or even a couple of years. So, the development of groin pain many months or even years after “pinning” and fracture healing can be caused by late femoral head collapse from AVN from loss of blood supply.
The actual trauma that results in breaking one’s hip imparts tremendous forces that not only results in bones breaking but also can damage hip joint cartilage. Even if the fracture heals and hip function is satisfactory restored, years later the hip may become symptomatic with groin pain from their hyaline cartilage progressively breaking down and ultimately developing osteoarthritis. Similarly, if the hip fracture heals but with less than perfect alignment or restoration of the anatomy (which is very common), then hip joint reactive forces are changed. The relationship of the femoral head to the socket (acetabulum) is changed and this too can lead to osteoarthritis years later with the development of groin pain.
If you’ve broken your hip and your doctor tried to help you with “pinning” the fracture with the hope that is would heal, and you’re having groin pain, recognize there are a lot of possible reasons that can have caused this. Some have better prognoses than others. If the pain is not improving and is interfering with your ability to remain active and fully engaged in life, then I would recommend you return to you surgeon for a full evaluation. If an etiology is not clear or further surgery indicated and you seek further opinion, then I suggest you consult with another orthopedic surgeon with a specialized interest and ability to address hip problems that occur after a hip fracture.
While I addressed the specific question of “groin pain after hip pinning” in this blog article, be aware that some individuals also develop hip/groin pain after a hip fracture treated with a replacement or endoprosthesis, and not a “pinning”. Again, there is a thought process, a work up and treatment options to address this, but I’ll save that for a future blog article.
Dr. William A. Leone is head of The Leone Center for Orthopedic Care at Holy Cross Health in Fort Lauderdale, Florida and has earned a reputation as one of the nation’s top orthopedic surgeons. An orthopedic surgeon with extensive experience, his specialty is solving complex hip and knee problems. We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4584 or by email at LeoneCenter@Holy-cross.com