Should I have both hips or knees replaced at the same time or separately? What if I don’t feel like coming back for the second procedure?
I see many patients who have arthritic symptoms from both their hips or knees, although one side is usually more painful or disabling than the other. This is because there is often an underlying genetic basis or predisposition that led to the arthritic destruction of the joint in the first place, such as dysplasia with hips or bowleg deformity with knees. Another consideration which helps explain why both sides are arthritic is that both lower extremities tend to be subjected to similar traumas, such as from sports.
Patients often ask me if they should have both their hips or knees replaced during one anesthetic session or would it be better to do the procedures in stages, first replacing the hip or knee that is most symptomatic and then replacing the other side after the original side has rehabilitated. Many patients then ask me if they stager their procedures will they feel like coming back for the other side.
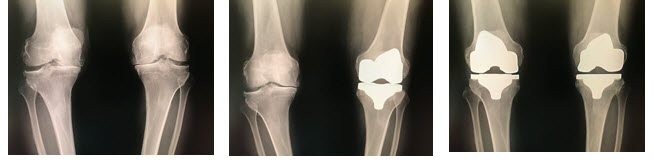
The x-rays below are from a 77- year-old, farmer from Illinois. He traveled to Fort Lauderdale for bilateral knee surgeries which were staged three weeks apart. This patient was disabled from severe degenerative arthritis of both knees and had bow leg deformities. He rehabilitated beautifully and flew home just several weeks after his second surgery, telling me he was so pleased that both of his legs looked straight!
To answer the last question first, I operate on numerous of people who return for their second side to be replaced. Many times I replace their second hip or knee just 3 or 4 weeks after their first surgery, and sometimes not until years later when their symptoms worsen enough to warrant replacement. For those who first present truly needing a bilateral procedure, we often schedule both sides as a planned, staged procedure. Some folks will not feel like returning just 3 or 4 weeks after their first surgery, but do so because “they just want to get it over with.” They can “see the light at the end of the tunnel” and are very confident after their first experience. If someone decides not to return for their second side, that is perfectly ok. In my experience however, the vast majority of my patients then do want their other side reconstructed because they’ve done so well with their first side.
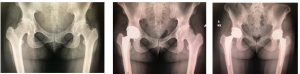
The x-rays below are from a 38-year-old teacher and mother with severe degenerative osteoarthritis secondary to underlying hip dysplasia. She had her left hip replaced first and her right three weeks later. She recovered beautifully!
Rehabilitating after a knee replacement, for most people, is more difficult and painful than after a hip replacement. The reason why so many patients these days are having their knees replaced in short succession is that at the Leone Center our surgery is better and our pain control is better. In prior blog articles, I discussed my use of computer navigation and use of the OrthoSensor to more consistently optimize alignment of the limb, congruency between the components and balancing of the soft tissue sleeve that supports the knee throughout the range of motion. In my experience, when knees (and hips also for that matter) are optimally aligned and balanced and soft tissue is gently handled, there is less swelling, less soft tissue trauma, motion returns more quickly and with less effort and less pain. Combined with our multimodal pain regime which is initiated before an incision is ever made, patients continue with strategies to decrease pain during and after surgery. This helps explain why my patients routinely walk the afternoon of their surgery and leave later that day or the next morning. Several years ago this simply was not the case.
So to again answer the question, if I have one knee or hip, replaced, will I come back for the other side, the resounding answer is absolutely yes.
Why do I encourage patients to stage their procedures rather than have both hips or knees replaced during one anesthetic session? I’ll preface my remarks by sharing that historically I replaced both hips or both knees for a patient during one anesthetic session routinely. The advantage was that it required only one hospital admission, the patient had only one uncomfortable period and healing process, and they would possibly be able to return to work or other responsibilities faster than if they had two procedures. I think all these are legitimate “historical” advantages. However, what I see today is that my patients are getting well so much faster than was feasible even a couple of years ago. They’re returning to their life’s responsibilities much faster, such as driving, working, and exercise. In earlier years, patients would take off from work for 6-12 weeks to rehabilitate both joints. Now, most patients who have a staged procedure resume work activities very soon after their first surgery (1-2 weeks) and again after their second surgery. Some patients elect to stay out longer, depending on their particular circumstances and needs.
Historically, patients stayed in the hospital after their surgeries much longer and almost all patients who had a bilateral procedure went to a rehabilitation facility. This pattern has radically changed because both health care workers and patients have come to realize that patients are safer and happier in their own environment at home. At home, they are once again “in charge” of their own health and must do more for themselves, which is therapeutic. Patients who go home rather than stay in the hospital or go to a rehab statistically have lower re-admission rates, lower complication rates, are subject to fewer medical errors. They are also happier. If someone is really sick, they need to be in the hospital; if they aren’t sick and just had their knee or hip replaced, they are much better off being home.
If a patient has a bilateral hip or knee replacement under one anesthetic setting, then they most probably will not be out of bed the day of their surgery and not walking. They almost certainly will not go home the day following their surgery and most will go to a rehabilitation facility rather than home, if their insurance will pay for it. Insurance companies including Medicare also recognize the medical and financial advantages of a patients’ early discharge from hospital to home rather than going to a rehabilitation facility. This has resulted in more insurance companies not approving, or greatly limiting, discharge options from the hospital to rehabilitation facilities. In other words, if discharge to a rehab is appropriate after a bilateral hip or knee replacement, the insurance company still may not approve it and if they do, the options may not include the facility of choice.
The risk of infection after a hip or knee replacement is thankfully extremely low, but not zero. I could not be more proud of our track record. The longer the time period an incision is open or the surgical instruments open to the environment, the higher the risk. Typically, the time interval that a bilateral hip or knee surgical field is open is nearly twice the time for a single side procedure and the same instruments are used for both sides. Some literature reports a higher infection rate after bilateral procedures, other literature does not substantiate this. In my mind, it’s an increased risk.
The need for a blood transfusion following a primary single side hip or knee replacement is extremely small. Not zero, but close. There is a much higher risk when performing a bilateral knee or hip replacement during one anesthesia. Again, this is a risk I prefer avoiding.
I counsel my patients who do need both their knees or hips replaced to replace first the most symptomatic side and then plan for replacing their other side in a “staged fashion”. Some people are eager to have both of their joints replaced quickly and then we plan their second reconstruction 3 or 4 weeks after their first. If they don’t think they are ready so soon after their first surgery, then we’ll delay until they feel that they are. Most do not delay.
Check out Dr. Leone’s Patient Testimonials. These grateful patients make it all worthwhile.
Dr. William A. Leone is head of the Leone Center for Orthopedic Care at Holy Cross Hospital in Fort Lauderdale, Florida and has earned a reputation as one of the nation’s top orthopedic surgeons. An orthopedic with extensive experience, his specialty is solving complex hip and knee problems. Call 954-489-4575 or email us to schedule a consultation.