Use of a Subcuticular Suture to Close Hip and Knee Incisions and Instructions for Suture Removal
Many patients ask me questions about where I will place the incision and how it will be closed. While there are a variety of methods which surgeons commonly use, including sutures (also called stitches), staples and even glue, I choose to close with a single subcuticular (or intradermal) non-absorbable suture. I prefer this method because it is gentle and very effectively seals the incision, which creates a barrier against infection and allows me to encourage patients to shower very soon after surgery. I also feel it produces the most visually pleasing scar. In fact, most plastic surgeons choose to close incisions using this subcuticular method. At The Leone Center for Orthopedic Care, we strive to make the incision appear as aesthetically pleasing as possible.
I care for many patients who travel to Fort Lauderdale specifically for surgery. Many will depart for home prior to having the suture removed. While they are given detailed instructions on wound care and suture removal prior to leaving, I’ve written this primer with embedded photos to give further instructions when it is time. Most patients have their orthopedic surgeon, primary care physician, rehab doctor, or nurse remove the suture once home. Many, but not all care givers are familiar with the subcuticular suture and the technique used to remove it. My hope is that this primer will help them.
Once the definitive total joint components are implanted, the tissues that support and surround the joint are anatomically closed to assure optimal healing and stability. Deeper tissues in the hip or knee are closed with absorbable sutures and therefore do not need to be removed.
The subcuticular suture is placed to hold the skin edges together until healing occurs and then is removed. This suture is woven through the edges of the skin with extra suture material left out of the skin on both ends of the incision to facilitate removal.
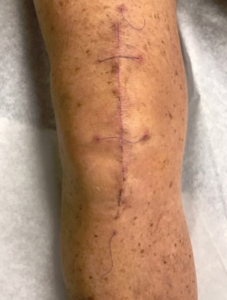
Often, we place one or more transverse suture loops, which when cut in the middle create a shorter length for easier removal.
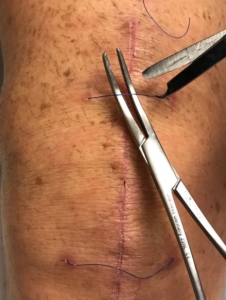
Typically, the subcuticular suture is removed 12 to 14 days after surgery. If there is concern with increased swelling or drainage, the suture can be left in the body for a longer period of time. Occasionally, a length of suture will break off during removal. The suture that remains in the body will create no problems and can be ignored.
Prior to suture removal, we recommend covering the incision with saline or hydrogen peroxide soaked gauze for about five minutes. This softens the skin and makes it easier to remove the suture. Any loops should be cut in half with scissors. The cut ends of the loop are cleaned with alcohol. Then, wrap the other end of the suture around a small instrument (a hemostat or needle holder works best) and apply a gentle pulling pressure. Continue to wrap the suture around the end of the instrument as the suture comes out of the incision. Apply gentle steady pressure aligned with the incision while holding the tip of the instrument close to the skin until the entire length of suture is free of the body.
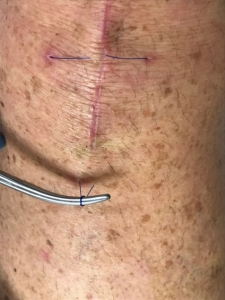
You will see the part of the loop that was cut disappear under the skin and eventually slide out completely. If there are any small gaps or open areas along the incision, keep clean with soap and water for a few days, allowing the body to heal itself.
We encourage our patients to shower after leaving the hospital and, one to two days after the subcuticular suture is removed, to start in-pool exercises, swimming or aquatic therapy if available.
Every incision should allow for the optimal placement of components with gentle soft tissue handling and balancing of the soft tissues, as well as recreation of proper leg length and alignment. Hip and knee replacement surgery is performed to relieve pain and restore quality of life, and critically important is the attention to detail beneath the incision. I believe this same attention to detail in performing the reconstruction must also be exercised when closing. While the length of an incision and a “great looking scar” are not substitutes for the best surgical outcome and recovery, it is reflective of the attention to detail below the incision and also is important.
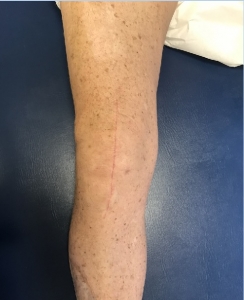
The patient’s incision four weeks post-op and two weeks post-suture removal
We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4575 or by email at LeoneCenter@Holy-cross.com.




great and helpful content..