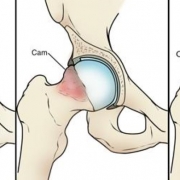
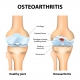
Hip and Knee Arthritis: Do PRP and Stem Cell Injections Work?
An estimated 50 million Americans have osteoarthritis (OA) . It is the most common cause of deterioration in hip and knee joints; the lifetime risk of being diagnosed with arthritis is 40% and one in two individuals will develop a symptomatic OA knee by age 85 years old.
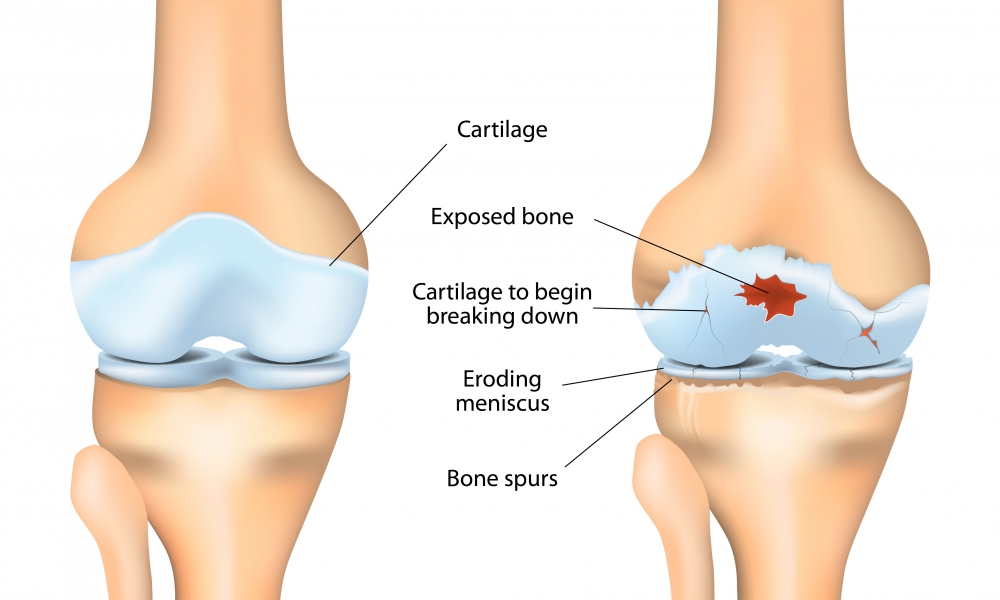
Osteoarthritis occurs when hyaline cartilage, a specialized tissue that covers the ends of the bones in a joint, is damaged and progressively wears away to the point of “bone on bone” friction. In a healthy joint, hyaline cartilage acts as a lubricant, decreasing friction and distributing joint reactive forces. Hyaline cartilage is not self-repairing and, when damaged progressively breaks down, resulting in pain, stiffness, diminished movement, and degrades one’s quality of life.
Once the degeneration of the cartilage lining a joint begins, it unfortunately progresses. Treatments to restore it are limited and reserved for early stage degeneration and joints with a limited area of arthritic disease. As the osteoarthritic condition progresses, it will deform the joint, alter the bone structure and compromise one’s independence and mobility.
Each of us has unique DNA which wholes the recipe and promise to re-create this special hyaline cartilage. There are numerous treatment options which try to harness or unlock our own cells ability to regenerate joint hyaline cartilage. There are legitimate methodologies which harvest our own cartilage cells to be grown or multiplied in a culture and then re-implanted. This is limited to small isolated areas of cartilage damage in knees (not approved for hip arthritis) and usually offered to young patients who have better healing potential. It is an expensive, time consuming process with a long recovery. It may be justified in a young individual with limited disease. This cartilage transplant treatment is not applicable when the cartilage damage is extensive or involves multiple areas of the knee. It is not applicable in the hip.
There are many dubious treatments circulating which claim to “cure arthritis,” such as with injections of stem cells or platelet-rich plasma. Let me address these.
Stem cells are naturally occurring cells in our body with the potential to develop into many different types of tissue including hyaline cartilage. Stem cells can be harvested from bone marrow, fat, and other tissues. An embryonic source, like the placenta can also be a source. The concentration of stem cells injected into an arthritic joint is often exceedingly small and the exact indications and protocols have not yet been determined. I believe these technologies do hold great promise for the future, but is now it is not a panacea and clearly can’t magically regenerate a joint which has advanced arthritis. This is “Tomfoolery”.
PRP (platelet rich plasma) is a concentration of the patients own platelets. It is obtained by drawing blood from an individual which is centrifuged, separating the red cells and concentrating the remaining the plasma which contain platelets and growth factors. Some PRP preparations are approved by the Food and Drug Administration (FDA) for some conditions but not for conditions of the hip or knee including OA. Some patients treated with PRP injections for OA of the knee do report pain relief and self-reported functional improvement. PRP concentrates have been demonstrated to have temporary anti-inflammatory properties.
Many reports regarding results after stem cell or PRP treatments are anecdotal. Specific indications, preparations, and protocols have not been standardized and agreed upon. Because treatments are considered experimental, health insurances do not pay for them. For many practitioners, this has resulted in an important “cash income stream” separate from insurance and regulation. Many practitioners with varying credentials and motivations are performing “their style” of stem cell and PRP treatments. Historically, because stem cells and PRP do not fall into a classic “drug” category, the FDA did not regulate them. The FDA more recently is getting involved and shutting down many of these facilities.
Nobody wants surgery, especially went there may be a potential alternative such as an injection that can delay or prevent it. I think this is understandable and completely reasonable. But I encourage anyone who is contemplating this treatment to become informed. There are established and agreed upon “conservative” treatments for hip or knee joint arthritis. When these treatments fail and one’s quality of life is effected enough (and this is a “personal” end point), then total knee (TKR) or total hip (THR) replacement may be appropriate. Sadly, this human instinct to avoid surgery is being exploited.
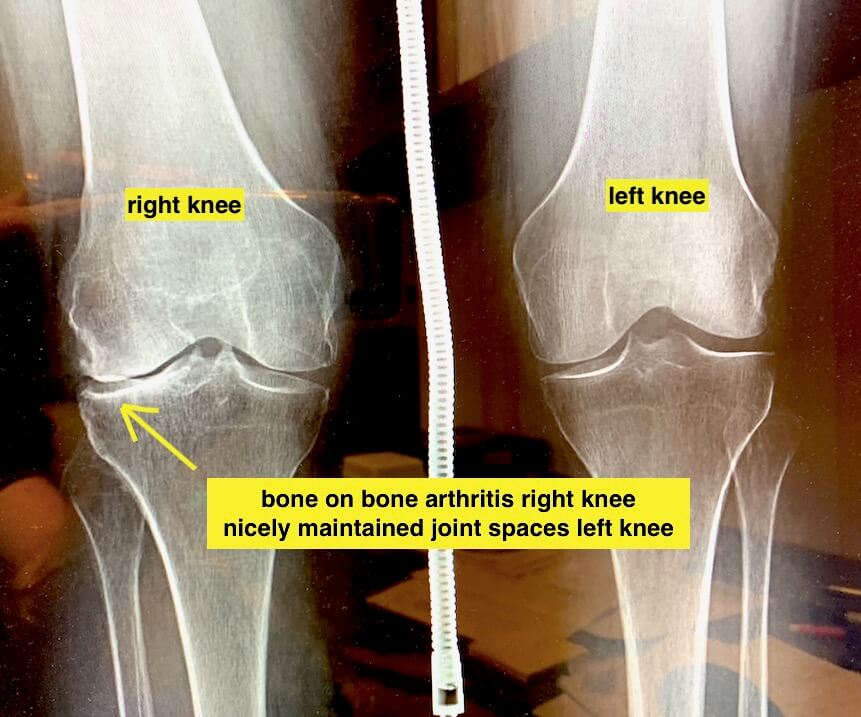
What none of these ‘’injections” can do is restore a severely arthritic joint. The disease process of OA is a continuum. Researchers and clinicians classify or “grade” the degree of OA destruction. The natural history of OA is that with time, the cartilage and underlying bone continues to breakdown resulting in the grade becomes higher. Major classifications progress from grade 0 to grade 4. When the joint space begins to narrow, i.e. cartilage loss is visible resulting in the bones becoming closer together and seen on an X-ray as “joint space narrowing”, that joint is classified as grade 2 or higher. Possibly these alternative treatment modalities like PRP and stem cell injections may be effective prior to joint space narrowing. They are clearly not effective for more advanced stages when all the cartilage has worn away and the bone are rubbing together (“bone on bone” or “end stage” OA). Possibly these treatments may temporarily relieve pain (like a cortisone injection) even with later stage OA, but will not magically result in cartilage growing back or restore a collapse joint space.
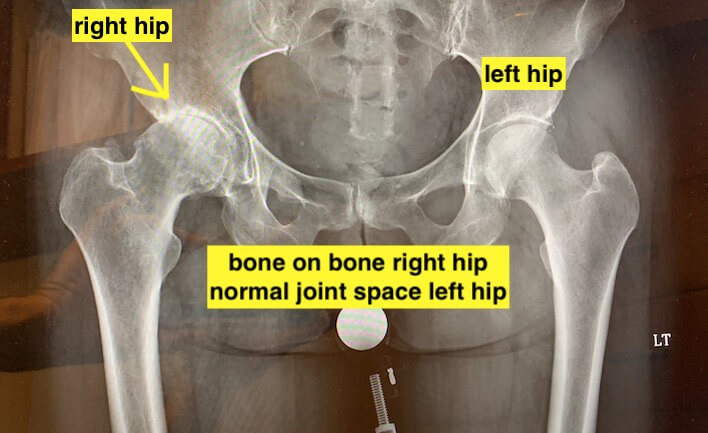
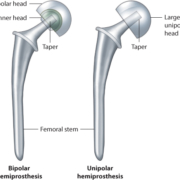
According to the American Association of Hip and Knee Surgeons, the largest association of hip and knee surgeons in the world, and closely associated with our American Academy of Orthopedic Surgeons, The Hip Society, The Knee Society and American Joint Replacement Registry, the most reliable and long-term solution remains joint replacement surgery. Partial and total hip and knee replacement surgery is a procedure where the diseased cartilage and bone of the joint are surgically replaced with artificial materials.
I frequently meet patients who have had many of these alternative treatments as well as others, prior to meeting me and then undergoing a hip or knee replacement. These novel treatments didn’t stop their arthritic disease process or relieve their symptoms in any lasting way and that patient still needed a joint replacement. They spent their time, personal money and invested their hopes and beliefs on these treatments, when to well informed practitioner, it was obvious their treatment was “doomed to fail from the beginning” and was no more than a “noble effort on their part”. It could not have possibly changed the natural progression of their disease and prevented their need for joint replacement in their future.
Unfortunately, in some patients not only are hopes dashed and money wasted but injury from these treatments can occur. This can greatly complicate caring for them with well-accepted and predictable treatments such as joint replacement. Infection or nerve injury can be devastating.
I have performed over 13,000 joint surgeries over the course of my career and am proud of The Leone Center for Orthopedic Care’s track record of superb clinical results, and the evidence backs that up. Performance data consistently demonstrates lower complications rates, infection rates, and readmission rates than peer orthopedists as well as shorter hospitalization stays and better patient satisfaction scores. More importantly, is the satisfaction of helping my patients becoming pain-free, regaining their mobility and enjoying life to the fullest. Don’t take it from me, click here to read some of the hundreds of patient testimonials my team has received.
Dr. William A. Leone is head of The Leone Center for Orthopedic Care at Holy Cross Health in Fort Lauderdale, Florida and has earned a reputation as one of the nation’s top orthopedic surgeons. An orthopedic surgeon with extensive experience, his specialty is solving complex hip and knee problems. We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4584 or by email at LeoneCenter@Holy-cross.com.