Medical Tourism: at What Cost? Having Hip or Knee Replacement Surgery Outside the U.S.
Several recent news articles have included interviews with patients who sought hip or knee replacement surgery outside of the U.S. Recently, medical tourism, where patients travel to other countries to offset the cost of having surgery, has come to the forefront. Many travel to the U.S. or other more medically advanced countries because the type of surgery needed is not always available where they reside. But for patients who travel outside of the U.S. because they seek lower overall fees, what is the real cost?
While surgical fees are a consideration, choosing where to have your hip or knee replaced is not like picking out an appliance or a new car. The success or failure of your surgery will have lasting effects on your health, lifestyle and mobility. The goal of so many of my patients, who are in their 60s, 70s and even 80s, is to remain very active, often with a desire to continue playing tennis, dancing, playing golf or even mountain climbing. I think all of these goals are wonderful and reasonable and I encourage my patients to return to full and active lives. In order to achieve this, both hip and knee replacement surgeries must be performed with leading-edge proven techniques, with the best prosthesis for each patient and the precision needed for optimum and long-lasting outcomes.
Before scheduling hip or knee replacement surgery outside of the U.S., ask yourself these questions:
• Can you fully evaluate surgeon and anesthesiologist credentials and licensing?
• How many hip or knee replacements has the surgeon performed and what are his/her successful outcome rates?
• Can you determine hospital accreditation and outcome data including infection rates, mortality rates and the legitimacy of the nursing and support staff?
• Is there accountability for the quality and consistency of care?
• Will the staff speak English and if not, how will you handle the language barrier?
• Is the quality and track record of the prosthesis transparent and accountable?
• Are replacement parts for the prosthesis available in this country, such as a new tibial plastic insert for a knee replacement or a femoral head or acetabular liner for a total hip replacement? Not uncommonly, foreign countries buy prosthesis that are not sold U.S. or use models that are not available here because they have not received FDA approval. Local manufactures also supply these prostheses and they might not meet the U.S. standard of approval. They might be cheaper, however, if non-standard or local implants are used, obtaining replacement parts is nearly impossible unless the patient travels back to country where surgery was performed.
• What if significant medical problems occur during or after surgery, such a heart attack, respiratory distress or failure, anesthetic overdose, urinary retention, etc.? Are there medical facilities, including an ICU, and a considerable support staff to address all medical emergencies? At Holy Cross Hospital, an intensivist is on duty 24 hours/7 days a weeks to respond to these emergencies. This, alone, has made a huge difference in patient safety and surgical outcome.
• How soon do you anticipate traveling after your surgery? Postoperative leg swelling and an increased risk of a blood clot (DVT) or pulmonary emboli must be considered. Will you be placed on anticoagulants? If so, which type, for how long and who will take over the responsibility of that care after you return home?
• How will rehabilitation and physical therapy after a hip or knee replacement be handled? Who will order additional therapy, if indicated, after you return to the U.S.? Some patients, in spite of their best efforts, struggle with regaining an adequate range of motion after knee replacement surgery. These patients might require a second procedure where anesthesia is administered and the knee is manipulated to break up early scar tissue. If this is necessary, who will perform this procedure? Will you be able to make arrangements with an American orthopedist willing to take on this responsibility and continue your care after you return home?
• If the procedure is done in another country, who will provide additional follow up? Even a patient with a well-functioning prosthesis requires periodic follow-up because wear and associated bone loss can develop silently.
• Have you considered that many doctors, especially in today’s medical climate, will not see or treat someone else’s patient, especially for a problem?
• After returning home, if you have a problem or concern, will you need to go back and see the surgeon who performed the procedure? If more surgery is needed, due to a prosthetic complication, is traveling back to that country something you really want to do or have planned for in your budget?
• Have you considered that if revision needs to be done for an infection or other reason, you may have no choice but to have it done in this country? Also, the treating physician might need to do a more extensive surgery — with further increased risks, complications and bone or soft tissue loss — because replacement prosthesis parts cannot be obtained from the country where you had the original surgery.
Every surgical procedure has risks and associated costs, but in the end it’s all about making a choice to put your health above all else.
We thank you for your readership. If you would like a personal consultation, please contact our office at 954-489-4575 or by email at LeoneCenter@Holy-cross.com.


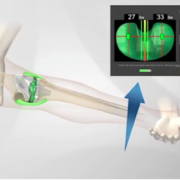


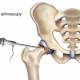
Thank you for your tips provided it was really helpful. Medical tourism, where patients travel to other countries to offset the cost of having surgery, has come to the forefront. Many travel to the India or other more medically advanced countries because the type of surgery needed is not always available where they reside.